Adult Nurse Practitioner definitions and practice questions.
Pinned to
64
0
0
No tags specified
|
|
Created by Annie Nguyen
about 9 years ago
|
|
Close
|
|
Created by Annie Nguyen
about 9 years ago
|
|

GI symptoms:
Abdominal pain, bloating, steatorrhea, abdominal distention and diarrhea
Systemic symptoms:
fatigue, weight loss, stunted growth, and muscle pain
Definitive diagnosis is made with IgA transglutaminase antibody test
Biospy performed by endoscopy or colonoscopy
DDX: irritable bowel disease
diverticulitis
gastroenteritis,
appendicitis
infection
food poisoning
medications side effect
metabolic disorders
gastrointestinal obstruction
Iron deficiency anemia
Early onset osteoporosis or osteopenia
Lactose intolerance
Vitamin and mineral deficiencies
Central and peripheral nervous system disorders
Pancreatic insufficiency
GI cancers
Gall bladder complications
Neurological manifestations, including ataxia, epileptic seizures, dementia, migraine, neuropathy, myopathy
A condition when undigested food causes pressure on the colon and forms a bulging pouch that pushes weak portion of colonic wall. Increased incidence with age.
This condition occurs near the distal portion of left colon, which is referred as sigmoid colon
Sign and Symptoms
Patient have localized mild to moderate pain in Left lower quadrant.
Frequent nausea and vomiting
Fever
Abdominal tenderness
Loose bowel movement or constipation
Complicated Diverticulitis
Occurs when colonic obstruction, frank perforation, intestinal rupture, abscess, fistula, or peritonitis developed
Uncomplicated Diverticulitis
Occurs when microperforation is limited to mesentery wall and pericolic fat and usually developed in sigmoid colon
Diagnosis is based upon the patient history and physical examination.
Blood test and blood culture reveals leukocytosis.
CT scan of abdomen is considered as best diagnostic test to confirm the diagnosis.
Endoscopy and colonography is avoided to prevent risk of perforation.
Conservative Therapy
Patient are admitted to the hospital for about a week to receive treatment for uncomplicated diverticulitis
Initial treatment includes bowel rest and maintain NPO status (nothing to eat or drink by mouth)
once patient started feeling better and have no abdominal pain NPO change to clear liquid diet
Advance to low fat and high fiber for 2 to 4 weeks
High fiber diet helps to firm the stool, regular bowel movement, resolve diarrhea and abdominal discomfort
Intravenous nutrition and fluids are administered to maintain nutrition, hydration and electrolyte balance until patient is able to tolerate per oral
Anticholinergic and antispasmodic agents are used during the course of treatment to relieve colon spasm
Demerol is used commonly for pain
Morphine is avoided due to the side effect of increasing colonic pressure
antibiotic therapy is very effective for outpatient treatment
ciprofloxacin and metronidazole 500mg BID X 7-10 days, Bactrim DS 160/800mg BID X7-10 days are commonly used or until the patient is afebrile for 3-4 days.
Surgical Intervention
patient with bowel obstruction or perforation need temporary colostomy
Typically laparoscopic surgery is done for colon resection, drainage of abscess, fistula repair or reversal of temporary colostomy
Immune-compromised patient are more prone for postoperative complications like slow wound healing
Patient with diverticulitis are encouraged to make numerous lifestyle changes to avoid flare-ups symptoms
Life style changes includes, avoid smoking, increase diet which are high fiber source, drink at least six to eight glasses of water, participate in regular exercise, avoid foods or medications that may causes constipation
Encourage patient to minimize fat in their diet and increase fiber rich diet like whole grains, legumes, high-fiber cereals, fruits, and green vegetables
High fiber diet helps to bulk stool, which reduce the incidence of constipation and prevent the formation of further diverticula, reduce abdominal discomfort, bloating, and flatulence.
Encourage patient to discuss their diet with their primary care provider so that provider can guide them correctly
Abdominal pain migrates to right lower quadrant and become more intense and localized. Appendicitis is the differential diagnosis of diverticulitis because in diverticulitis pain is in the lower abdomen but more intense and localized in the left lower quadrant, where sigmoid colon is located
Colorectal cancer also resembles the symptoms of the generalized lower abdominal pain, fatigue, weakness, weight loss, alternating diarrhea and constipation. Colorectal cancer is differential diagnosis of diverticulitis because colonoscopy will be positive, colonoscopy is necessary for biopsies, positron emission tomography (PET) scan is additional diagnostic test detect tumor origin and metastasis
common disorder that affects the large intestine (colon). IBS commonly causes cramping, abdominal pain, bloating, gas, diarrhea and constipation. IBS is differential diagnosis of diverticulitis because IBS improved with defecation, onset change in stool frequency, form and appearance.
1) Diverticulitis is an inflammatory response of obstructed diverticulum and increased pressure on diverticulum due to obstruction leads to perforation of diverticulum
A) True
B) False
2) Complicated diverticulitis is when micro perforation is limited to mesentery wall and peri colic fat.
A) True
B) False
What is the recommendation for patient with diverticulitis to prevent flare-ups symptoms?
A) Drink plenty of water
B) Eat high fiber diet
C) Quit smoking
D) Only A & B
D) All of the above
Diverticulitis commonly occurs at long intestine in
A) Ascending colon
B) Descending colon
c) Sigmoid Colon
D) Transverse Colon
5) Which pain medication is avoided due the side effect of increasing colonic pressure in diverticulitis?
A) Morphine
B) Demerol
C) Dilaudid
D) Tylenol
the chronic GI functional disorder characterized by abdominal discomfort or pain with altered bowel habits in the absence of a specific and unique organic pathology
Affects the large intestine (COLON).
abdominal pain or cramping,
having a bloated feeling, gas, diarrhea/ constipation
mucus in the stool
visible distention and bloating in some cases
Abnormal Motility,
Constipation-predominant irritable bowel syndrome (IBS-C)
Diarrhea-predominant irritable bowel syndrome (IBS-D)
Visceral Hypersensitivity,
Enteric infection
Psychosocial Abnormalities
depression, anxiety, panic attacks and hypochondriasis
made by the physical examination and the presenting clinical signs and symptoms
The Rome III diagnostic criteria
recurrent abdominal pain or discomfort for at least 3 days/month in the last 3 months associated with at least one or more of the following symptoms
improvement with defecation,
onset associated with a change in frequency of stool,
onset associated with a change in form or appearance of stool
If the patient presenting with the signs and symptoms of IBS but has a positive family history intestinal cancer, inflammatory bowel disease, or celiac disease then he or she has to undergo further evaluation
Adolescence : Incidence Increases
Third and fourth decades it peaks
Affects women more than men
Symptoms after age 50 is unusual, and should consider obtaining a colonoscopy, if not already performed
rritable bowel syndrome is a chronic condition
Managing the symptoms with pharmacologic treatment should be viewed as being adjunctive rather than curative
making the symptoms diary, and knowing the stressors either medication, dietary or psychosocial as it helps manage the symptoms and increase adherence to treatment plan
Stress may trigger Irritable Bowel Syndrome.
Causes :
Irregular bowel habit from repeated inhibition of normal defecation reflexes.
Overuse of laxatives for prolonged periods.
Due to slow colonic transit (more in women)
Defecatory disorders (more in women)
Endocrine disorders
Hypothyroidism
Hyperparathyroidism
Diabetes mellitus. Metabolic disorders
Hypokalemia
Hypercalcemia Neurologic conditions (causing gut dysfunction & myopathies)
Parkinsons
Multiple Sclerosis
Sacral nerve damage (prior pelvic Sx, tumor)
Paraplegia
Autonomic neuropathy
Structural abnormalities that can cause constipation
Anorectal abnormalities-prolapse, stricture, fissure, ulcer
Perineal descent
Colonic mass with obstruction- adenocarcinoma
Colonic stricture- radiation, ischemia, diverticulosis
Hirschsprung disease
Idiopathic megarectum
Most commonly reported symptoms:
Hard stools
Excessive straining
Fewer than 3 stools/week
Feeling of not having a complete evacuation
Associated symptoms include-
bloating
fullness, abdominal pain
Symptoms r/t specific causes
Rectal pain or bleeding- with hemorrhoids, fissures
Decrease in diameter of stool- in intestinal obstruction
Nausea, polyuria, fatigue- in hypercalcemia
DRE- may identify stricture of anus, rectocele, rectal prolapse, perineal descent, abnormal pelvic floor motion
Presence of Rome III criteria symptoms confirms constipation.
Physical Examination
Auscultate bowel sounds
Assess tympani to evaluate stool in the colon
Palpate abdomen for tenderness & masses
Digital Rectal Exam (DRE )
to palpate hard stool, assess masses, hemorrhoids,
anal fissures,sphincter tone, prostatic hypertrophy in
men, push effort, posterior vaginal masses in women
Common Radiologic Exam / Imaging
Abdominal plain X-Ray (KUB)
Helpful in detecting significant stool retention
May suggest diagnosis of megacolon
Barium enema
To identify areas of colon dilatation & obstruction
Endoscopic Examination - to r/o malignancy
Colonoscopy / Flexible sigmoidoscopy
Indicated in pts with alarm symptoms
Special Procedures
Radiopaque marker methods
Most commonly used – to measure colonic transit time
Abdominal radiograph is performed 120 hrs after ingestion of 24 radiopaque markers
If it shows retention of >20 %, prolonged colonic transit is indicated.
Inadequate fluid intake & medications are the main
causes for constipation
Thorough H&PE–initial step in elderly assessment
Digital rectal exam (DRE) –
very significant in elderly presenting with loose stools
Fecal impaction may result in overflow incontinence causing loose stool
Bulking agents can worsen constipation in elderly
who do not consume adequate fluids
Mineral oil can cause aspiration pneumonia
Prophylactic treatment is beneficial for elderly at
high risk for fecal impaction
Dietary modification
Increase dietary fiber in normal transit constipation
Fiber rich foods and fiber supplements
Decreases colonic transit time
Increases stool bulk
Sufficient fluid intake -daily
3L(thirteen 8oz )for men, 2.2L (nine 8oz)for women
30ml/kg bodywt daily for pts taking Bulking agentsDietary modification
Low residue diet is recommended for patients with refractory slow transit constipation and with pelvic floor dyssynergy
Fiber can worsen symptoms in pts with defecatory disorders, colonic inertia, opioid induced constipation , and Lifestyle modification
Increasing physical activity and exercise
Attempting defecation at particular times
Colonic activity is stimulated during waking up
in the mornings/meals
Probiotics
Promotes colonic mucosal health
Lactobacillus may improve constipation
Bulking agents
Stool softeners and emollients
Osmotic laxatives
Stimulants
Chloride secretory agents
Opioid-receptor antagonists
First line agents for constipation
Help to produce softer stool
They expand with water->Increases bulk of stool
->Softens stool
Ex- psyllium, calcium polycarbophil,
methylcellulose
C/I- patients with swallowing difficulty,
possible rectal mass/bowel obstruction,
those who do not consume adequate fluid.
Have a detergent effect on the stool consistency
Ex- docusate, mineral oil
Use mineral oil with caution in elderly-
can cause aspiration & lipoid pneumonia
Used when bulking agents or stool softeners
are not effective
Increases secretion of water into the intestinal lumen-->
softening of stools and stimulation of defecation
Ex- polyethylene glycol(PEG)—>considered best.
Lactulose, sorbitol, magnesium hydroxide
Increases peristaltic contraction, increases intestinal motility, Results in a BM 6-12 hrs after ingestion.
Melanosis Coli-marker for chronic laxatie use seen on colonoscopy assoc. with stimulant laxatives.
Chloride secretory agent.
stimulates intestinal chloride secretion, increase intestinal fluid, and accelerates colonic transit. last line. ex. lubiprostone and linaclotide
Blocks peripheral opioid receptors of the GI tract, reverses opiod induced peristalsis inhibition, mostly used in pallative care.
ex. methylnaltrexone, mu-opiod receptor antagonist.
Teaching r/t drug therapies (contd)
Fiber should be taken 1 hr before or 2 hr after other medication since fiber may inhibit drug absorption
Onset of action varies with laxative types
PEG (Miralax) and Magnesium hydroxide preparations are not recommended for those with CHF and Chronic renal disease – may cause electrolyte imbalance
Irritable Bowel Syndrome- less seen in >=50 yrs
Recurrent abdominal pain / discomfort- improved upon defecation
Intestinal Obstruction
Progressive constipation associated with pain and nausea, marked abdominal distention, reduction in BM frequency, thin “pencil” stool, palpable mass, pain/tenderness
Colon Cancer- more in > 40 yrs
Unexplained constipation associated with abdominal distention, colicky pain, weight loss, anorexia, decrease in laxative effect, blood/pus/mucus in stool.
Which one of the following is included in Rome III criteria used by clinicians to define constipation?
Straining during all defecations.
Loose stools are rarely present without use of laxatives.
Hard or lumpy stool in more than 20% of all defecations.
Fewer than 4 defecations per week.
The estimated prevalence rate of constipation in individuals older than 65 years is:
25%
30%
40%
45%
Melanosis coli is associated with the use of:
Stimulant laxatives
Osmotic laxatives
Bulking agents
Stool softeners
None of the above
Which one of the following is linked with aspiration and lipoid pneumonia in older adults?
Magnesium citrate
Lactulose
Sorbitol
Mineral oil
A chronic inflammatory condition of the bowel
One of the inflammatory bowel diseases (IBD)
Affects the mucosal inner lining
of the colon and rectum,
resulting in inflammation and
ulceration
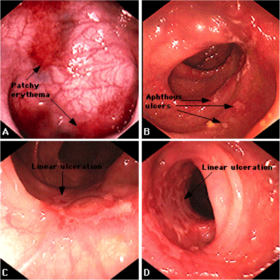
The appearance of inflamed colon is characterized by
Edema
Hyperemic
Granular
Mucopus
Friability
Erosion
Wide range of ulcerations tend to
Cause normal mucosal areas to look
like polypoid, called psuedopolyp
The disease can be
Limited only to recto-sigmoid area, called proctosigmoiditis
Expanded to the splenic flexure, called left sided colitis
Expanded proximally, called extensive colitis
The signs and symptoms of UC
Diarrhea with blood or pus
Abdominal pain and cramps
Rectal pain and bleeding
Urgency to defecate
Loss of weight
Severe tiredness
Anemia
Fever
Most of the population experience sudden onset of symptoms
and a period of remission
(McPhee & Papadakis, 2014)
In the United States
About 2 million people are affected
Ages 15 – 30 are more frequently affected
Men and Women are equally affected
UC is exacerbated by
Use of NSAIDs
Intake of less antioxidants (Vitamin A & E)
Psychological stress
Alcohol
Smoking
Intake of milk products
Proper and accurate history collection
Physical Examination
Abdominal and rectal examination
Labs
Stool tests
Complete blood count (CBC)
Erythrocyte sedimentation rate (ESR)
C-reactive protein (CRP)
Electrolytes
Albumin and Liver function test (LFT)
Imaging- in severe colitis
Abdominal plain X-rays - to look for colonic dilatation
Barium enema studies are in limited use, induce toxic megacolon
Endoscopy
Sigmoidoscopy can be done in acute colitis – to look for abnormal changes in mucosal lining
Colonoscopy should be avoided in severe colitis – risk of bowel perforation
Main Objectives - to decrease symptoms and to continue remission.
Anti-inflammatory drugs- first line of treatment: Aminosalicylates (Sulfasalazine, Mesalamine, Balsalazide, Olsalazine)
Help to decrease symptoms of UC
Available in the form of suppository, enema, and oral
Corticosteroids (Prednisone, Hydrocortisone)
Used to treat moderate to severe UC, if other treatment is failed
Available in the form of oral, intravenous, enema, and suppository
Not advised for long term use- increased and dangerous side effectsImmune system suppressors
To control immune system response, thereby reducing the inflammation
Azathioprine (Azasan, Imuran) and Mercaptopurine (purinethol, Purixam)
Broadly used by providers to treat IBD
Regular follow-up and blood works are necessary to look for side effects
Cyclosporine (Gengraf, Neoral, Sandimmune)
Used if other treatments are failed
Not for long term use due to serious side effectsInfliximab (Remicade), Adalimumab (Humira), and Golimumab (Simponi)
Used for moderate to severe UC if other treatments are failed or not tolera
Antibiotics
To prevent or control infection if fever presents
Anti-diarrheal
Used with caution due to risk for developing toxic megacolon
Lopramide can be used for severe diarrhea
Pain relievers
Tylenol can be used for mild pain
Avoid NSAIDS- exacerbate the disease
Iron Supplements
To prevent iron deficiency anemia due to chronic ble
Maintenance therapy
UC patients who are on remission period to prevent reoccurrence
Oral aminosalicylates are commonly prescribed
If patient treated with infliximab, need to be continued with infliximab or azathioprine.
Indicated for patients who are unresponsive to medication therapy
Unmanageable toxic megacolon
Unmanageable intestinal bleeding
Prolonged use of steroids
Dysplasia or adenocarcinoma
Avoid alcohol and smoking - to prevent worsening of symptoms
Take medications regularly as prescribed (CCFA, 2015)
In active diarrhea, avoid dairy products, spicy and fatty foods, and high fiber foods – aggravate the symptom (Wedro, 2015c)
Eat well balanced and nutritious diet - to prevent weight loss
Frequent Colonoscopy studies - to detect signs of cancer
Adequate exercise, calcium and vitamin D supplements
To prevent osteoporosis due to prolonged corticosteroid therapy
Which of the following is considered as an inflammatory bowel disease (IBD)?
a. Celiac disease
b. Diverticulitis
c. Infectious colitis
d. Ulcerative colitis
2. Which symptom is the hallmark in ulcerative colitis (UC)?
a. Bloody diarrhea
b. Constipation
c. Dysuria
d. Vomiting
Which age group of people are more commonly affected by UC?
a. 15 - 30 years
b. 35 - 45 years
c. 40 - 60 years
d. 50 - 75 years
4. Which of the following drug class is the first line of treatment in UC?
a. Analgesics
b. Antibiotics
c. Anti-inflammatory
d. Immunosuppressant
In severe UC, the following diagnostic tests are performed except
a. Abdominal X-ray
b. Colonoscopy
c. Labs
d. Physical examination
Originates from a growth of non-cancerous tissue or tumor, usually a polyp on the inner lining .
Adenomatous polyps are pre-cancerous cells.
85% of adenomas turns into cancer.
Hyperplastic and inflammatory polyps are not pre-cancerous, but may increase the risk of adenomas.
A family history in 20% of patients
When cancer cells are detached from their primary source, they invade into nearby blood or lymph vessels and can travel to distant parts of the body, a process called metastasis
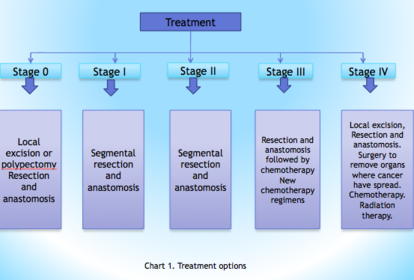
Stage 0 (Carcinoma in situ) – Cancer has not grown beyond the inner layer (mucosa) of the colon.
Stage I - Cancer has grown through the muscularis mucosa.
Stage II - Cancer has grown into the outermost layers of the colon or rectum.
Stage III – Cancer has outgrown the wall of the colon. Invasion into lymph vessels. Beginning of metastasis.
Stage IV – Cancer has spread to peritoneum and distant parts of body.
Change in bowel habit
Diarrhea or constipation
Blood in stool
Feeling of fullness in the rectum
Unusual narrowing of stool
Bloating, cramps or gas pain
Unintentional weight loss
Fatigue
Anemia
LABS
A complete blood count (CBC) may detect anemia.
Liver function tests to rule out liver metastasis.
Carcinoembyronic antigen (CEA)
levels can detect prognosis
and extent of the cancer.Fecal Occult Blood Testing (FOBT) examines the stool for hidden blood that occasionally sheds from adenomatous polyp sand cancer.
Fecal Immunochemical test (FIT) detects antibodies specific to human globin in the stool. Colonoscopy-
Gold standard, cost effective,
reliable.
Permits biopsy for pathologic
Confirmation of malignancy.
CT colonography- Two and three
Dimensional views are taken
Through colonoscopy.
Flexible sigmoidoscopy
Looks inside the rectum and
sigmoid colon. Only a portion of
distal colon is examined.
Computed Tomography
Looks beyond the intestinal layers.
Most useful in detecting metastasis
Barium enema –
Liquid barium sulfate and air is
inflated into the inner part
of the colon and rectum followed
by x-rays to look for obstruction
Local excision and polypectomy are done at stage 0 and early stage I, can be done through colonoscope.
In Colectomy, the cancerous segment of the colon as well as immediate lymph nodes is removed through an abdominal incision also termed as resection and anastomosis.
A temporary or permanent colostomy is made for fecal diversion .
Works well and safe
Shrink or slow the growth of tumors and reduce pain.
Adjuvant chemo is given after the
surgery to shrivel the remaining cancer cells.
Neo adjuvant chemo is done before surgery to shrink the cancer and make surgery easy to manage.
In target therapy, drug stops the action
of molecules that aid the growth of cancer.
Works differently from chemotherapy and
less side effects.
Aimed when the cancer has adhered to an adjacent internal organ or the inner layer of the abdomen.
May be used before, during and after surgery to shrink the tumor and reduce the risk of recurrence.
Most often, it is used in stage IV to alleviate symptoms in people with progressive cancer causing intestinal blockage, bleeding, or pain.
Tests that detect adenomatous polyps and cancer
Colonoscopy every 10 years
Flexible sigmoidoscopy every 5 years
Double contrast barium enema every 5 years
CT colonography every 5 years
Tests that primarily detect cancer
FOBT every year
FIT every year
Stool DNA test every 3 years
A well-balanced diet.
Increase fruits and vegetables, and reduce the fat, particularly animal fat.
Maintaining body weight, exercise and physically active lifestyle.
Quit smoking.
A low dose aspirin a day can lower the chances of developing polyps, especially in patients with previous history of polyps or colorectal cancer
1. Most reliable, preferred and cost effective diagnostic test to detect colon cancer is
Sigmoidoscopy
Barium enema
Colonoscopy
Labs and Fecal Occult Blood Test
2. One of the recommendations from the Society of Geriatric Oncology (SIOG) in regards to the treatment goal for elderly is
To provide the most intensive and applicable treatment thought to be safe and potent to their biological age and comorbidities.
Treat them like young patients.
Treatment is very limited as there is usually risk for complications in elderly.
Maximize the survival rate even though complication arises
3. What is metastasis?
Cancer cells detached from primary source and attaches within five inch of primary source.
Cancer cells detached from primary source and travels to distant parts of the body.
Cancer cells detached from primary source and infiltrates in the liver.
Cancer cells detached from primary source and forms of an obstructive mass.
. According to the American Cancer Society, colonoscopy should be done
Beginning at age 50, every ten years.
Beginning at age 45, every ten years.
Beginning at age 50, every year.
Beginning at age 60, every ten years.
hile educating your patients on colon cancer, you will explain them to watch for which of the pertinent colon cancer symptoms?
Change in bowel habit, weight gain and headache.
Diarrhea with abdominal pain for two – three days.
Belching and heartburn.
Change in bowel habit, dark and narrow stool, fatigue and unusual weight loss.
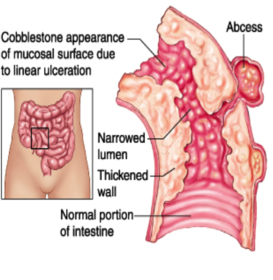
A chronic recurrent gastrointestinal disease characterized by patchy trans mural inflammation that can involve any part of the GI tract from the mouth to anus.
Most prevalent in Northern states compared to Southern states in the United Sta an autoimmune disease targeting GI tract
Peaks age is 15-40 years old
Hereditary tendency
CD results from an abnormal immune response, producing tissue damage and inflammation through all layers of the GI tract-such as abscesses, perforation and ulcerations.
BILATERAL LOWER QUADRANT PAIN
INSIDIOUS ONSET
FEVER
CHRONIC DIARRHEA
WEIGHT LOSS
FATIGUE
MALNUTRITIONS
ABDOMINAL DISTENTION AND OR MASS
Assess for other autoimmune related symptoms such as: joint tenderness, swelling or psoriatic lesions
Detailed medical/family history
Rule out other diseases that may mimic CD such as: C. difficle, lactose intolerance and celiac disease
#1 diagnostic procedure is a upper/lower endoscopy with biopsies of mucosa to rule out H. pylori or cancer
Fact: 10% of cases difficult to distinguish ulcerative colitis from CD. Biopsies that contain granulomas highly suggest CD diagnosis.
CT or MRI: to visualize bowel thicken, tissue perfusion and r/o appendicitis
Labs: CBC, CMP, ESR
Stool cultures: test and rule out pathogens such as C. difficle, E. coli, ova and parasites
Nutritional management
Well balanced diet-low fat and low roughage diet
Understand food triggers
Smaller meals, adequate water
Vitamins B-12, probiotics
Lifestyle modifications
Cessetion of all tobacco use
Nutritional management
Well balanced diet-low fat and low roughage diet
Understand food triggers
Smaller meals, adequate water
Vitamins B-12, probiotics
Lifestyle modifications
Cessetion of all tobacco use
10-15% new diagnosis in patients older than 65 years old
Less likely to present with normal symptoms and present with more weight loss, oral ulcers and anemia
Correct diagnosis often delayed to due presenting as other disease processes and not as common in elderly
Increased mortality when first diagnosed age 60 or greater
Medication dosage may need to be reduced due to decreased GFR, hepatic elimination
Common to see noncompliance due to other disease processes
Avoid NSAID/ASA
Understand not curable and management only
Smoking cessation is imperative
Emotional support important
Nutritional management huge factor with triggers
Need to have regular physicals, gastroenterologist and colonoscopy's often
Which of the following stool characteristics would be present in a client diagnosed with Crohn’s disease?
a. Chronic Constipation
b. Diarrhea with alternating constipation
c. Normal stool
d. Chronic Diarrhea
Which factor is thought to be linked to Crohn’s disease?
A. BMI
B. Lack of exercise
C. Genetics
D. Gender
Which associated disorder may the patient with CD present with?
A. Malabsorption
B. C. difficile
C. Celiac disease
D. Lactose deficiency
When diagnosing a patients with CD its important to educate to follow which type of diet?
A. High fat-low roughage diet
B. Low fat-low roughage diet
C. Low carbohydrate diet
D. No change
l
Which of the following areas of the gastrointestinal tract is affected in CD?
A. Only the rectum
B. The small bowel and colon
C. The colon
D. The small bowel
Spirochete multiplys and systemactically spread.
S/S. more diffused lymph nodes involvement, fever, hadache, nausea, rashes and joint pain.
more central neurologival symptoms appears, such as anemia, jaundice and stiff neck, or meningitis and deaf.
The spirochete eventually spreads to central nerves system, muscular skeletal system, and cardiovascular system.
Syphilis encephalopathy resulted.
Primarily focused on complete sexual history.
S/s from physical exam.
Serolgic tests. includes none treponemal tests and treponemal test
Treponemal tests: Venereal Diesase Research Laboratory(VDRL) and Rapid plasma reagin test( PPR)
are to detect the presence of antibodies. often fives out false positive
usually used for first line screening.
Direct tests: Darkfield microscopic examination.
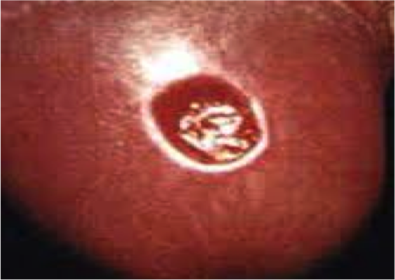
1st: Plainless chancre sore and lymphadenopathy
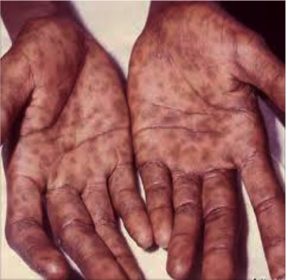
2nd: Rashes over soles and palms, joint pain and stiff neck.
3rd: Cencephlopathy
Penicillin G 2.4 million unit,IM.
,or Docycyline 100mg BID for 4 days.
,or Ceftriaxone 1g IM for 10 days.
Penicillin G 2.4 million unit for 3 weeks.
Tertiary syphillis:
Penicillin G , IV, q 3 to 4 hours for 14 days and then daily for 3 weeks.
educations for the usage of protective sex, such as condoms.
prevention is more important than treatment.
high risk people need to be screened more frequently, every 3-6 months.
HIV pt also need to be screened for syphillis.
At what stage of syphilis can neurosyphilis occur?
A. primary syphilis
B. Secondary syphilis
C. Early latent syphilis
D. any state of disease
Which of the following is true regarding the progression of syphilis?
a. the most common clinical manifestation of primary syphilis is a chancre at the site of inoculation.
b. mucocutaneous lesions may occur during secondary syphilis.
c. tertiary syphilis is rare.
d. all of the above.
Which of the following is true about primary syphilis?
A. a pailful chancre occurs at the site fo inoculation.
B. the chancre is generally pailess and resolves without treatment
C. Nontreponemal serologic tests are always postive.

 Hide known cards
Hide known cards