Flashcards on Muskuloskeletal Exam 1, created by cristydlhz on 01/02/2014.
|
|
Created by cristydlhz
over 10 years ago
|
|

What is the Roentgen sign approach? (p 85)
List the five opacities
What could result in changes in soft tissue size?
List the different kinds of osteolysis and rate them in increasing order of aggressiveness:
What is the difference between short and long zone of transition?
What do the different bone margin lines mean? I.e., if they are easy to trace, irregular, or very irregular?
Characterize the zone of transitions in order of aggressiveness.
Characteritize the nerve supply in the articular cartillage
HOw many layers in joint capsule:
What is the purpose of the synovial fluid
What is purpose of articular cartillage
What is the purpose of the ligaments
What is the meniscus and what does it do?
Can you characterize Degenerative Joint Disease (DJD)? What are other names for the conditions, what species are affected, etc?
What species are affected by DJD?
What is DJD/What can DJD be secondary to?
What are common radiographic signs of DJD?
What are occasional radiographic signs of DJD?
What are uncommon radiographic signs of DJD?
How can you use the infrapatellar fat pad to evaluate synovial volume?
Describe the evolution of osteoarthritis.
What is the purpose of ostephytes? Where do they occur?
Do osteophytes occur within or outside a joint capsule?
What are enthesophytes?
What can enthesophyte formation b secondary to?
How are osteophytes and enthesophytes different?
What are some intracapsular mineral bodies? (Will go over a few in other lectures)
What is synovial osteochondrosis?
What is the process of synovial osteochondromatosis?
What is subchondral bone sclerosis?
Subchondral Bone Cysts
What is joint space widening and why does it occur?
What are five critical components to diagnosing lameness?
What kinds of questions do you ask during a history?
What kinds of questions should you be asking during a history?
In a general physical examination, remember to:
Gait Analysis: What should you do in general
Gait Analysis: Distinguish between walk, trot, and pace
What is the most important gait for evaluating lameness?
How to do you evaluate gait?
What do you look for in a gait analysis when studying forelimb?
For forelimb lameness, does head bob when weight on lame leg or normal leg?
What are you looking at when evaluating hind limb lameness?
Quantify lameness by utilizing the 0-4 scale.
During a visual inspection (gait analysis) to evaluate lameness, what are you looking for in terms of conformation?
During visual inspection (gait analysis/lameness), what are you looking for in? (Posture and few others)
During a visual inspection (gait analysis/lameness), where would you look for areas of muscle atrophy?
What is the general purpose/what do you do for palpation (for gait analysis/lameness) ?
Valgus
Varus
For lameness examination, where would you palpate?
For lameness exam and during palpation, what does swelling of knee joint on medial aspect mean?
What can you do to check for lumbosacral disease?
To localize lameness, do you start with or without sedation?
What other examination do you do along with orthopedic exam?
What are two important rules for localization (when trying to identify lameness)?
How would you localize lameness during orthopedic examination.
What is an specific Orthopedic Test?
What is the Ortolani Sign--how do you know it?
Please describe another orthopedic test: Cranial Drawer
Can you please describe another orthopedic test: Tibial Compression Test
Can you please describe the orthopedic test: Patella luxation
What are the goals of a specific orthopedic examination?
Why would you need to perform a sedated orthopedic examination?
Why would you need to perform a radiographic assesment (for orthopedic exam/lameness section)?
What is involved with client communication (for orthopedic examination/)
1. How are joints classified? Give examples of joints that fit into each category.
What is the function of the synovial joint (aka diarthrodial joint)?
What is the synovial joint composed of? What is their purpose?
Please characterize the different layers of the synovial joint and the vessels and nerves:
Describe the two types of synovial cells:
What is the synovial membrane composed of?
What is the function of the synovial membrane? How can it be damaged and what results?
2. What are the components of the synovial joint and what are the functional roles of each component in maintaining joint health?
What does normal synovial fluid look like?
What are components of the synovial fluid? Where is synovial fluid located?
What are Synovial fluid functions ?
What does articular cartilage look like? Where is it?
What are some components of articular cartilage?
Characterize hyaline cartilage:
Characterize proteoglycans (as part of the articular cartilage structure)
Charactertize GAGS (articular-cartilage structure):
In terms of the articular cartilage, what are some functions of the proteoglycans and GAGS?
Characterize hyaluronan (in articular-cartilage):
What separates Zone 3 and Zone 4 in articular cartilage?
What are the different zones of articular cartilage (basic):
Please characterize zone 1 of articular cartilage:
Charactertize zone 2: transitional zone (of articular cartilage0
Characterize zone 3 of articular cartilage:
Characterize zone of calcified cartilage in ariticular cartilage.
What are the functions of articular cartilage (joint)
What is the meniscus made of and what is its function?
What is weeping lubrication?
What happens to fluid during compression (movement)
Joint Movement and Lubrication: What happens? Leading Edge/Trailing Edge.
For joint lubrication/movement: what is the difference between collagen fibrils and proteoglycans in terms of load sharing?
What is subchondral bone? What does it do?
What would result in abnormal joint motion?
What is an articular fracture? What is the goal?
What should you do for long bone fractures? (Joint Function/Structure PPT)
What is hip dysplasia?
Cartilage Injury and healing: Characterize superficial lacerations and healing
Charactertize full thickness defects in cartilage injury and healing:
What is bicipital tenosynovitis? Please characterize it. How can we visualize it?
Which are lateral and which are medial?
Biceps brachii, supraspinatus, greater tubercule, infraspinatus
What kind of radiographic view will you take for BICIPITAL TENOSYNOVITIS?
What radiographic findings might you encounter with BICIPITAL TENOSYNOVITIS?
What is polyarthropathy?
What are the two types of polyarthropothy?
Characterize non-erosive polyarthropothy:
Between erosive and non-erosive polyarthropathy, which does not cause articular damage?
Characterize erosive polyarthropathy. What species tend to be afffected?
Is Rheumatoid arthritis erosive or non-erosive polyarthropathy?
Is Feline periosteal proliferative arthritis erosive or non erosive? (Polyarthropathy/polyarthritis)
What radiographic findings might you find with erosive polyarthritis?
Characterize septic arthritis: What animals does it occur in, adults vs juveniles
What is the process of septic arthritis?
What are some characteristics of joint associated tumors?
What are the locations for joint associated tumors? (possibly from most common to least?)
What are some differentials for joint associated t umors?
How do you differentiate between erosive polyarthritis, septic arthritis, and joint neoplasia from each other?
Monoarticular problem--how do you characterize disease? (Picture with how to figure out what kind of aggressive disease you have)
Polyarticular problem--how do you characterize disease? (Picture with how to figure out what kind of aggressive disease you have)
From Lecture 5, this is a flow-chart of characterizing Arthropathies in Dogs and Cats (Two categories). Draw it out.
1. Define the term osteoarthritis.
Characterize osteoarthritis:
Difference between ankylosis and arthrodisis?
What is difference between primary and secondary osteoarthritis?
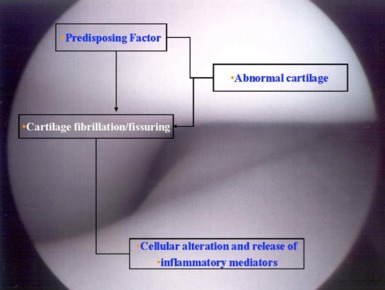
2. What is the pathophysiology of osteoarthritis
3. What are the typical history and clinical signs/findings in patients with joint disease?
What are some Radiographic Findings for Osteoarthritis?
What are five basic principles for treatment of joint disease?
In terms of treatment of joint disease, how does weight management help?
Each level above the target level (for dog's body condition score) represents X percent excess body weight.
What is one inciting factor for OA (in terms of weight management) ?
What is the difference between arachidonic acid and dihydroxyeicosapentaenoic acid?
Treatment of Joint Disease: Nutritional Supplementation: What is a major supplement (lots of evidence for)?
Treatment of Joint Disease: Nutritional Supplementation: Examples of weak nutrient supplementation (not used so much)
Treatment of Joint Disease: Nutritional Supplements: What re some of the benefits of Chondroprotectives/DMOA
What are some examples of chondroprotectives and how do they work?
Treatment of Joint Disease: Supplement: Chondroprotective. Be careful of what?
What are some contraindications for chondroprotectives?
Can you characterize the chondroprotective pentosan polysufate?
Treatment of Joint Disease: Controlled Exercise: Purpose and how do you approach this?
Treatment of Joint Disease: Physical Rehabilitation Therapy: What does it do? How does it work? Benefits?
Treatment of Joint Disease: Medical Therapy: What kinds of therapy would you use?
Treatment of Joint Disease: Medical Therapy: What is most commonly used agent? What are benefits of this?
Treatment of Joint Disease: NSAIDS inhibit XXX
Treatment of Joint Disease: NSAIDS: Use Ibuprofen and Naproxen?
Treatment of Joint Disease: Example of COX Non-specific NSAIDS
Treatment of Joint Disease: Examples of COX-2 Preferential NSAIDs
Treatment of Joint Disease: NSAIDS: Examples of COX-2 selective
Treatment of Joint Disease: NSAIDS: Cox and Lipoxygenase inhibition
Treatment of Joint Disease: NSAIDS: List Counterindications
Treatment of Joint Disease: NSAIDS: Counterindication for Carprofen
Treatment of Joint Disease: NSAIDS: Counterindication for Keratoconjunctivitis
Treatment of Joint Disease: Steroids: What do they do? Include counter indications
Treatment of Joint Disease: Other Potentially useful agents: Analgesics
How can you diagnose septic arthritis?
How do you medically manage septic arthritis? What are your options?
Septic Arthritis: Medical Management: Describe antimicrobial therapy : When? How long?
Treatment of Joint Disease: Non-Erosive Polyarthritis: Idiopathic Immune Mediated. How would you treat?
Treatment of Joint Disease: Non-Erosive Polyarthritis: Systemic Lupus Erthematosus
Treatment of Joint Disease: Erosive Polyarthritis: How would you treat rheumatoid arthritis?
Treatment of Joint Disease: Erosive Polyarthritis: How would you treat feline chronic progressive polyarthritis?
Treatment of Joint Disease: Discuss surgical treatment
Treatment of Joint Disease: Please describe the cycle that must be interrupted in order to treat osteoarthritis
How does normal bone develop? (Normal Bone development)
How does longitudinal bone growth occur?
1. What is endochondral ossification?
What happens to chondrocytes in the former proliferative zone of articular cartilage and the diffuse zone of calcified cartilage during endochondral ossification?
What is osteochondrosis (OC)?
Which growth plates can osteochondrosis affect?
Osteochondrosis: Pathogenesis: Characteristic the disturbance of endochondral ossification
Briefly talk about the pathogensis of osteochondrosis:
3. What is the difference between osteochondrosis (OC) and osteochondritis dissecans (OCD)?
What is the separation between non-calcified and calcified layers called?
Osteochondrosis: What can happen with the cartilage flap?
What are causes of osteochondrosis?
Causes of osteochondrosis: Characterize Trauma
Osteochondrosis Etiology: Characterize Anatomical Factors
Osteochondrosis Etiology: Characterize Hormonal Factors
Osteochondrosis: Etiology: Characterize over nutrition
Osteochondrosis: Etiology: Characterize Rapid Growth Rate
Osteochondrosis: Etiology: Characterize heredity:
Osteochondrosis: Etiology: Characterize ischemia
Ischemia (Abnormal Blood vessels) has been noted in which species:
Osteochondrosis: Etiology: Characterize lipid metabolism
When is period of rapid growth in dogs?
How would you diagnose OCD?
5. What breeds are commonly affected by OC ?
True or False: Is OCD bilateral?
What is the signalment, usually, for dogs affected with shoulder OC? And where is the subchondral bone defect?
When looking at a shoulder, what are you looking for to confirm shoulder OC? Subchondral bone defect!
What clinical signs will you see with a dog who has shoulder OC?
How do you treat a dog with shoulder OC? Discuss the options
Discuss medical management of dog with shoulder OC: Age?>?
Discuss surgical management in a dog with shoulder OC:
What is the typical signalment of elbow OC in a dog?
Where do you typically find/look for defect for shoulder OC in dog?
Where do you typically look for Elbow OC in dog?
What are clinical signs of elbow OC?
What is a tip-off that dog has elbow OC?
How would you medically manage elbow OC?
How do you medically treat elbow OC?
7. List the joints and specific anatomical locations within the joints where OC is commonly seen.
8. What is the incidence of OC in the joints that are commonly affected?
What are clinical signs of stifle OC?
What is a difference in clinical signs for stifle OC?
Describe medical management in stifle OC
Describe surgical management in stifle OC:
Characterize Hock OC: Signalment
What breeds are typically affected by hock OC?
(Osteochondrosis lecture): A hind limb lameness in a large breed dog is usually:
What are clinical signs of hock OC?
Where do you tend to see Hock OC?
How would you clinically manage HOCK OC?
How would you surgically manage HOCK OC?
What is the prognosis for Shoulder OC?
What is the prognosis for elbow oC?
What is the prognosis for stifle OC?
What is the prognosis for tarsus OC?
What is the prognosis for various Joint OC?
In general, how do we treat OC?
What is to "forage"? (OC lecture)
What is the general surgical treatment for OC?
Compare arthrotomy and arthroscopy:
Talk about the prognosis for shoulder, stifle, elbow, and tarsus osteochondrosis
Where can the OATS procedure be applied?! (OS)
What is the OATS procedure?
For OS surgery (osteochondrosis), what are some post-operative care consideratiins and what are some complications?
Juvenile Bone Disease: What are some radiographic signs for OC?
What is a kissing lession?
Juvenile Bone Disease: How can you distinguish OCD and OC?
Juvenile Joint disease: What are common sites of OC (canine)?
Is Fibula lateral or medial?
Is radius medial or lateral?
What are some developmental conditions that lead to elbow DJD? (Elbow Dysplasia):
For Juvenile Bone Disease: What breeds are at risk for Ununited Anconceal Process?
What are the Roentgen Signs for a dog with ununited anconeal Process (UAP)
What does Ununited Anconeal Process look like?
What kind of view would you take to look at ununited anconceal process in a dog? And is this uni or bilateral (the condition)?
Juvenile Bone DZ: Characterize fragmented medial coronoid process
What are some Roentgen signs associated with fragmented medial coronoid process?
How many physis does the ulna have?
Radius/Ulna Asynchronyous Growth (Elbow Dysplasia):
How manny physes does ulna have? What about its growth?
What happens with premature ulnar physis closure?
What is ULNAR OSTECTOMY?
Characterize premature radial physis closure:
Characterize Panosteitis: What breeds get it? Which bones affected?
Age range for dogs that develop panosteitis?
What are early Roentgen Signs for dogs with Panosteitis?
What are late Roentgen signs of Panosteitis?


Characterize hypertrophic osteodystrophy (HOD): What breeds, age, etc?
What are the Radiographic findings for HOD (hypertrophic osteodystrophy)?
What are the three different stages for HOD (Radiographic findings): Hypertrophic osteodystrphy
What is a key radiographic finding to HOD (HYPERTROPHIC OSTEODYSTROPHY (HOD)
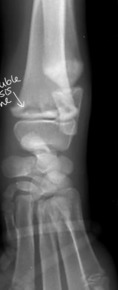
What is retained cartilaginous core?
What are radiographic signs of retained cartilaginous core?
What is the most common cause of hind limb lameness in the dog?
What are the three types of cranial cruciate ligament ruptures?
Functions of the CCL
What is the typical signalment for an animal with CCL rupture?
What is the etiology for CCL rupture?
Characterize the etiology of acute trauma and chronic degenerative changes for CCL rupture:
Charactertize conformation abnormalities as as a cause for CCL rupture
For CCL rupture, how do you distinguish between acute and chronic injury and partial tears?
If you hear a click during walking or on stifle flexion, this is suggestive of:
What may you find during physical examination of dog with CCL rupture?
Craniomedial and craniolateral band in CCL
True or False: Fractures usually require blocking
What are some symptoms for fractures of the 3rd phalanx? (P3)
What is one way to diagnose P3 fractures?
Be slightly be familiar with P3 Fracture classification.
How would you treat P3 fractures? This depends on the type of fracture.
Treatment for Type 4 fracture on P3?
What is the prognosis for P3 Fractures?
What is a common etiology of 2nd phalanx fractures?
How would you diagnose 2nd phalanx fractures?
How would you apply first-aid to horse with a P2 fracture?

 Hide known cards
Hide known cards
